
Facts
- Brain tumours are the most common form of solid tumours among children.
- Brain cancer kills more children in Australia than ANY other disease.
- Brain cancer survival rates are low and have hardly changed in over three decades.
- Treatment is challenging because it affects a human beings most vital organ.
- On average, approximately 1750 brain cancers are diagnosed each year in Australia; that is roughly one person diagnosed with brain cancer every five hours. (Australian Institute of Health and Welfare (AIHW) 2017)
- Brain cancer costs more per person than any other cancer.
- Only two in ten people diagnosed with brain cancer will survive for at least five years. (AIHW 2017. Cancer survival and prevalence in Australia)
Symptoms
- Persistent or recurrent vomiting often on waking
- Abnormal or poor balance
- Wobbly or gaited walk
- Poor co-ordination
- Unexplained weight loss or gain
- Behaviour change
- Fits or seizures
- Abnormal eye movements and blurred or double vision
- Lethargy
- Abnormal head position such as a head tilt or stiff neck
- Delayed or arrested puberty in adolescents
- Reduced consciousness
- Diabetes insipidus (excessive drinking and urination)
- Frequent flu like symptoms
- Decline in school performance
- Loss of bowel or bladder control
More information
A brain tumour is a mass of unnecessary and abnormal cells growing in the brain. There are two basic kinds of brain tumours:
- primary brain tumours
- metastatic brain tumours.
Brain tumours are categorised according to where the tumour originated, its pattern of growth and whether it is benign or cancerous. The tumour is also graded by its degree of malignancy and its chances of growing and spreading. There are now approximately 130 different types of brain tumour. Names of the more common varieties include: gliomas (astrocytomas, glioblastomas, oligodendrogliomas, ependymomas and mixed cell type gliomas) meningiomas, medulloblastomas and central nervous system lymphomas.
Brain tumours can be benign or malignant. Malignant brain tumours are also called brain cancer.
Primary Brain Tumours
A tumour that starts in the brain is a primary brain tumour. Primary brain tumours may be grouped into “benign” and “malignant” tumours. Glioblastoma multiforme (GBM), astrocytoma, medulloblastoma and ependymoma are examples of primary brain tumours.
A benign tumour consists of very slow growing cells, usually has distinct borders, and rarely spreads. Treatment and/or surgery is often effective, however, if a benign tumour is located in a vital area of the brain, it is life-threatening.
Malignant brain tumours vary widely both in the way they grow and the way they respond to treatment. Some are neatly contained within a capsule (encapsulated) and relatively easy to remove. Others have long, thin filaments spreading through the brain, like the roots of a plant.
Benign Tumours:
- Slow growing
- Distinct borders
- Rarely spreads
Malignant Tumours:
- Usually rapid growing
- Invasive
- Life threatening
Metastatic Brain Tumours
Metastatic brain tumours begin as cancer elsewhere in the body and spread to the brain. All metastatic brain tumours are malignant since they begin as cancer elsewhere in the body. Most common metastatic brain tumours start in the lung, breast, colon (bowel), or skin (melanoma).
Paediatric Brain Tumours
Children are different to adults: their bodies and brains are still developing. Their tumours are different too. The most common childhood brain tumours are not the same as the most common adult brain tumours.
Brain tumours are the most common form of solid tumours among children under the age of 15. Yet they remain the most difficult to cure.
Childhood tumours frequently appear in different locations and behave differently than brain tumours in adults. Treatment options vary depending on the type of tumour and age of the child. The treatment of paediatric brain tumours is more complex than that for other childhood cancers. Surgery to remove the tumour is not always possible because it may be inaccessible or because surgery would cause too much damage to the surrounding brain tissue. prognosis for children diagnosed with brain tumours depends not only on the type, grade and size of the tumour, but on its location in the brain

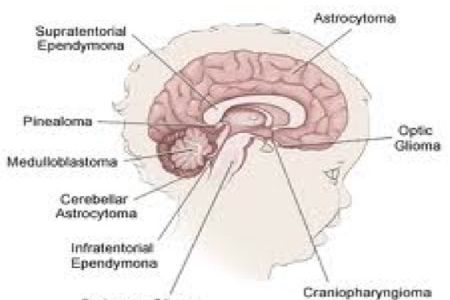
Over 60% of childhood brain tumours are located in the posterior fossa, the lower region of the brain. This includes the cerebellum and the brain stem. Tumours in this area include Medulloblastoma, cerebellar astrocytoma, brain stem Glioma and ependymoma.
The remaining 30 to 40% of brain tumours occur within one of the two cerebral hemispheres or in the spinal column. Tumours of the hemispheres include astrocytoma, craniopharyngioma, choroid plexus papilloma, ependymomas and germ cell tumours. The most common tumours of the spinal cord are astrocytomas and ependymomas.
Brain stem gliomas are a group of tumours located in the area of the brain called the brain stem. These account for 10% of all brain tumours in children and commonly affect children between the ages of 5 and 10. They can be low or high-grade, however a larger number (70%) are high-grade.
The brain stem is the area of the lower back portion of the neck which connects the spinal cord with the brain. It is the area of the brain and spinal cord that is responsible for many of the body’s vital functions, including vision, swallowing, gagging, balance and strength. Because of the location of these tumours, they are more difficult to treat than tumours in other parts of the brain.
Low-grade brain stem gliomas are focal, or confined to one area while high-grade brain stem gliomas tend to be diffuse, or infiltrate and spread throughout the brain stem.
Children with low-grade brain stem gliomas commonly present with a long history (greater than 6 months) of symptoms including:
- Headaches
- Vomiting
- Visual disturbances
- Unsteady, clumsy walk
Low-grade brain stem tumours may be partially or incompletely removed, despite being located in a vital area of the brain. This is because they are generally contained to one area of the brain stem. Additional treatment such as chemotherapy and/or radiotherapy following surgery is often not required. Chemotherapy may be necessary in children whose tumour progresses following surgery or whose tumours are not surgically accessible.
High-grade brain stem tumours (DIPG) because of their location within the brain stem which is diffuse and infiltrating cannot be surgically resected. Surgery in this situation could lead to damage to the nerves within the brain stem that are vital for breathing, swallowing, consciousness, arm, leg and eye movement. A biopsy is rarely performed for similar reasons. Therefore diagnosis is often made on clinical presentation and an MRI.
Radiation treatment to the area of the tumour is the current standard treatment for this tumour type. A large percentage of children will clinically improve with radiation, but their condition will decline rapidly within 6 to 9 months after completing therapy. There is currently no clear role for chemotherapy in the treatment of these tumours.
Medulloblastoma (PNET) is the most common brain tumour of childhood, representing about 20% of all paediatric brain tumours. They are most common in children between 4 and 10 and are slightly more common in boys than girls.
These tumours typically arise in the middle of the cerebellum, interfering with the flow of cerebrospinal fluid and causing hydrocephalus. Medulloblastoma is highly malignant and aggressive and can spread to other parts of the brain and spine through the cerebrospinal fluid.
Common symptoms include:
- Vomiting (most common) with/out nausea, most often in the morning after
- Waking
- Headaches
- Clumsiness
- Difficulty with tasks like handwriting
- Gradual decline in school performance (impaired attention)
- Unusual sleepiness or change in energy level
- Change in personality or behavior
- Unexplained weight loss or weight gain
If there is spread to the spinal cord symptoms may include:
- Back pain
- Difficulty walking
- Problems with bowel and bladder control
Treatment for Medulloblastoma is usually surgical removal, followed by high doses of radiation of the entire head and spinal cord and high dose chemotherapy with stem cell rescue.
Medulloblastoma is classified as low or high risk with lower survival rates for high risk patients and a greater chance of a recurrence.
Recurrent Medulloblastoma has long been considered universally fatal. In spite of attempts to improve its treatment, only rarely have long term survivors been documented in the world’s medical literature, there is no established treatment for its recurrence.
Ependymomas arise from the cells that line the brain’s fluid spaces, known as the ventricles. These represent about 10% of all brain tumours in children. About 60% of children diagnosed with ependymomas are under 5. Like other brain tumours, the cause remains unknown.
Ependymomas commonly occur in the posterior fossa (lower back of the head) part of the brain but can also occur in the top part of the brain, known as the cerebral hemispheres.
Symptoms of tumours in the posterior fossa include:
- Vomiting and nausea due to increased intracranial pressure
- Headaches
- Unsteady walking
Symptoms of tumours in the cerebral hemispheres include:
- Visual disturbance
- Headaches
- Possible seizures
Ependymomas, like other brain tumours are diagnosed by MRI, however a biopsy is necessary to confirm this. Other tests such as a lumbar puncture can help in staging the disease.
Tumours that arise in the posterior fossa are more often difficult for the neurosurgeon to completely remove compared to those that occur in the top areas of the brain. This is because they have the tendency to spread into the vital part of the brain known as the brain stem. This is a delicate part of the brain that must be preserved.
Following surgery to the posterior fossa, children over the age of 4 will receive localised radiotherapy to the original location of the tumour and a small margin surrounding it. These children do not require further treatment other than frequent MRI scans to monitor for recurrence. Children who have partial or incomplete removal of their tumour will receive a course of chemotherapy following radiation treatment.
When ependymomas arise in the top part of the brain, the neurosurgeon is generally able to remove the entire tumour without causing damage to the surrounding tissues. In this group, no additional therapy is performed and the child undergoes regular MRI scan to monitor for recurrence.
Astrocytomas are tumours that arise from brain cells called astrocytes. Gliomas originate from glial cells, also called astrocytes. The terms are often used interchangeably. Astrocytomas account for the majority of childhood brain tumours. In children more than 80% of astrocytomas are low-grade and 20% high grade.
Low-grade astrocytomas are usually well localised and grow slowly over a period of time. High-grade astrocytomas tend to grow rapidly and infiltrate healthy brain tissue surrounding the tumour. These tumours require more intensive treatment.
The signs and symptoms children present with or continue to experience are dependent upon the location of the tumour and the age of the child. The most common area for these tumours to occur is within the cerebellum, above the back of the neck.
Symptoms include:
- Headaches
- Vomiting and nausea occurring most commonly in the morning
- Changes in coordination
- Unsteady, clumsy walk
Less frequently these tumours occur in the cerebral hemispheres (left and right) at the top of the brain. Children may experience:
- Seizures
- Weakness in arms and legs
Children who present with a tumour in the area of the optic nerve and hypothalamus often present with:
- Visual disturbance (decrease in vision and double vision)
- Hormone problems
- Headaches
- Arm and leg weakness
Tumours are graded according to how serious and advanced they are. Tumour grade is assigned based on the tumour’s microscopic appearance using some or all the following criteria:
- similarity to normal cells (atypia)
- rate of growth (mitotic index)
- indications of uncontrolled growth
- dead cells in the centre of the tumour (necrosis)
- potential for invasion and/or spread (infiltration) based on whether or not it has a definitive margin (diffuse or focal)
- blood supply (vascularity).
Most doctors now use the World Health Organization (WHO) classification system to grade brain tumours.
WHO Grading System
Grade I Tumour:
Slow-growing cells
Almost normal appearance under a microscope
Least malignant
Usually associated with long-term survival
Grade II Tumour:
Relatively slow-growing cells
Slightly abnormal appearance under a microscope
Can invade adjacent normal tissue
Can recur as a higher-grade tumour
Grade III Tumour:
Actively reproducing abnormal cells
Abnormal appearance under a microscope
Infiltrate adjacent normal brain tissue
Tumour tends to recur, often as a higher grade
Grade IV Tumour:
Abnormal cells which reproduce rapidly
Very abnormal appearance under a microscope
Form new blood vessels to maintain rapid growth
Areas of dead cells (necrosis) in centre
While some types of brain tumours can be treated, many remain lethal. Even within the tumour types for which current treatments have the greatest success, many tumours display resistance to current treatments and subsequently relapse, and currently there is no way to predict which children this will happen to. Treatment for childhood brain cancer/tumours may involve:
- Surgery
- Chemotherapy
- Radiotherapy
- Steroids may also be given to decrease the swelling caused by the tumour
- Autologous Stem Cell Transplant
A child may undergo some or all of these treatments, depending on their tumour type and grade, the child’s age, overall health and medical history, and family preferences.
As with other tumours in both children and adults, surgery is the primary treatment, usually followed by radiation treatment and/or chemotherapy.
Unfortunately, because a child’s brain is still developing, these treatments can result in more substantial and permanent side effects than they would for an adult. Sadly, not all brain tumours can be treated with surgery, diffuse tumours in the brainstem (for example, DIPG) surgical removal is not an option.
If a child receives radiotherapy, it is given in a lower dose than is used for adults and is rarely used for children under the age of three. This is because it can slow physical growth and intellectual development.
Better treatments are urgently needed, and the key to this is a better understanding of the biology of brain cancer cells. This information can then be used to develop innovative and highly selective treatments for all paediatric brain tumours.
Often children can have access to Clinical Trials, this is a link to assist: https://clinicaltrials.gov/ct2/results/refine?recr=Open&age=0
A prognosis for a child diagnosed with a paediatric brain tumour greatly depends on:
- The type of tumour
- The extent of the disease
- Size and location of the tumour
- Presence or absence of metastasis
- The tumour’s response to therapy
- The child’s age and overall health
- The child’s tolerance for specific medications, procedures or therapies
- New developments in treatment




