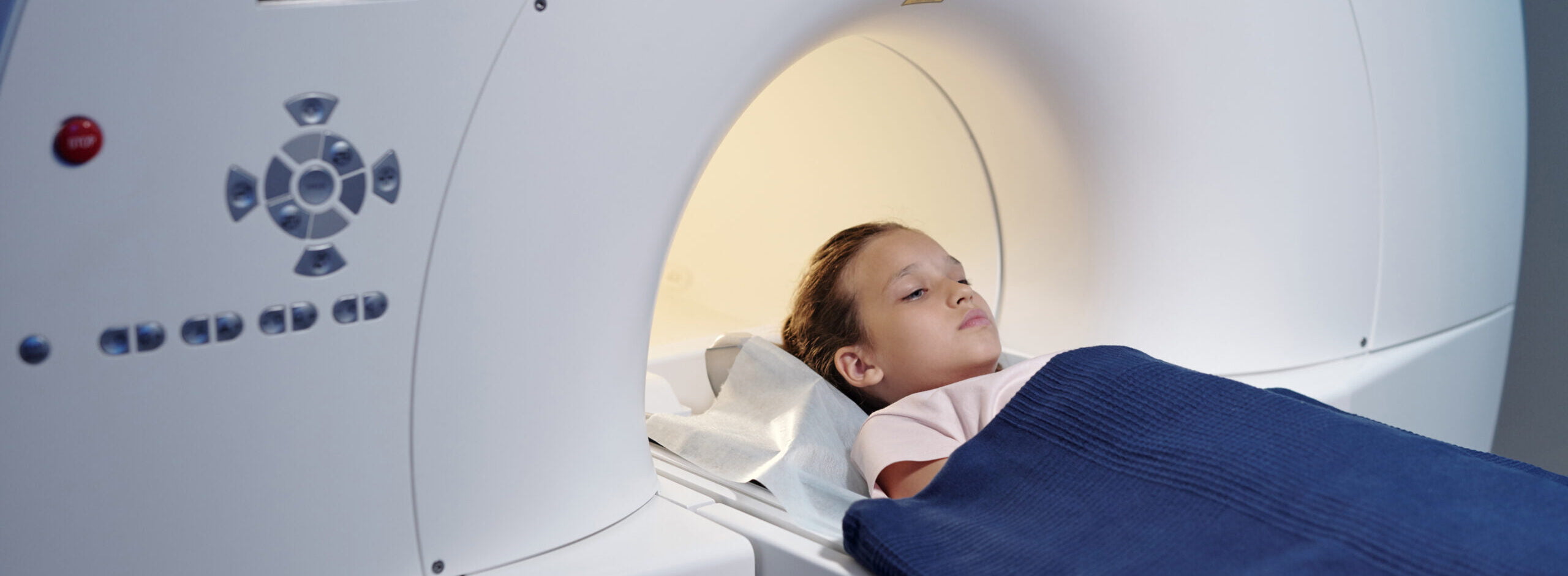

Procedures and Scans for Children With Brain Cancer
If a paediatrician suspects a child has a brain tumour, they’ll usually begin by examining brain function. This is often a neurological examination to inspect speech, hearing, vision, and movement function. It may include checking reflexes, balance, and coordination, testing muscle strength, the ability to feel sensation, and sometimes simple brain exercises such as memory tests.
The paediatrician may also use an instrument called an ophthalmoscope which enables them to view the optic nerve and examine eye and pupil movements. The optic nerve sends visual information from the eyes to the brain. This is important, as swelling of the optic nerve can be an early sign of increased pressure in the skull, possibly from a tumour.
A child is then sent for an emergency MRI at the local hospital.
MRI scans use radio waves and magnets to create an image of the inside of the body. An MRI machine is shaped like a long, narrow tube.
An MRI can provide information about the body that other scans may not be able to. MRIs are used to:
- detect abnormal growths, including tumours, in the body
- help determine the stage of a tumour (how big it is and whether it has spread)
- help the doctors decide on the best treatment.
Your child or sibling will need to lie very still on a table that slides into the tube. The actual MRI is painless however, being in a confined space could be a little distressing. The machine also makes loud noises, which can be scary or overwhelming for kids.
However, your child or sibling can wear earplugs or headphones to help block out these noises. They can also take in a favourite CD which the technician can play for them. A soft toy can also be taken in as long as they have no metallic parts. A parent can stay for support, they must remove all jewellery and wear earplugs.
Infants or young children may be given a sedative (medicine to calm them down and help them stay still) and others may be given a general anaesthetic so that they sleep through the test.
MRI scans take longer than X-rays or CT scans, it could take an hour or more, an MRI of the just the brain is shorter than one of the brain and spine, so sometimes these are done on separate days.
Contrast agents are often given before an MRI scan, which can make different parts of the body stand out better in the image. These are usually injected and can cause some discomfort.
A lumbar puncture is also often called a ‘spinal tap’.
Brain cancers can spread into the fluid around the brain and spine. This fluid is called cerebrospinal fluid (CSF). A doctor will use a lumbar puncture to collect the CSF.
A lumbar puncture involves a needle that is inserted into the lower back, between the bones of the lower part of the spine (also called the lumbar spine), to remove a sample of CSF. This procedure takes around 20 minutes.
Lumbar punctures are extremely painful and can be traumatic. For this procedure your child or sibling needs to stay very still.
However, depending on age and to avoid such stress the doctor may choose to give them either:
- a general anaesthetic, to put them to sleep so that they don’t feel any pain, or
- another medicine for ‘conscious sedation’, where they will be awake during the procedure but will not feel pain.
They will need to lie on their back for up to an hour after the procedure to reduce the chance of developing a headache.
A pathologist will look at the sample under a microscope to determine whether the sample contains cancerous cells. Part of the sample may also be sent to a laboratory to check for tumour markers. It will usually take a few days for you to find out the results.
A child with brain cancer will have many blood tests. Blood tests are also used to check for general health and organ function.
To do a blood test, the doctor will insert a small needle in your child’s or sibling’s arm (usually in a vein on the inside of their elbow). The doctor will collect a small amount of blood to be tested in a laboratory. The blood test shouldn’t be painful but might be cause a little discomfort initially.
If they have a port-a-cath or central line, then this accessed to take, which can be much easier and less stressful.
Finger prick blood tests or Capillary Blood Sampling is another way of taking blood. It is for smaller blood tests, where up to 2mls is required. The finger is pricked with a small handheld device. Blood is collected into small collection tubes. Sometimes they must squeeze the finger to get enough blood out and this can be uncomfortable.
Sometimes EMLA Cream can be used before a blood test. This is a cream that numbs the skin and can be very effective, it needs to be applied to the skin 25–45 minutes before the procedure.
Blood samples need to be sent to a special laboratory to check them. It can sometimes be a few days before you find out the results. The most common blood tests are a full blood count and blood chemistry.
A blood transfusion is a way of giving a small amount of one person’s blood to another person who needs it. During treatment for brain cancer your child or sibling may require numerous blood and blood product transfusions.
You may be wondering what the different blood components are. Blood has different parts, and each part has a job to do. The components are: Red Blood Cells – carry oxygen around the body. They are given during brain cancer treatment because it causes anaemia (low numbers of red blood cells). Platelets – are cells that help to stop or prevent bleeding. Plasma – is used to help blood form a clot. It may be used with platelets to prevent or stop bleeding. Albumin – is a protein in the plasma and can be given to help increase the albumin levels if they are low within the blood. Albumin levels are important to maintain, as they keep fluid in the blood stream.
It is interesting that before a transfusion is given to your child or sibling, two nurses or medical staff will carefully check that the details on the blood pack match the details on the order and your child’s or sibling’s wrist band.
The transfusion is usually given through a central line, port-a-cath or an IV (commonly referred to as a drip/cannula).
One pack of blood is called a unit and it can take up to 4 hours to be given. Sometimes your child or sibling will need more than one unit of blood. During the transfusion time a nurse monitors the process very closely.
Childhood Brain Cancer treatment can affect your child’s or siblings’ heart so a procedure that is regularly done is an echocardiogram or echo. An echocardiogram is a test that uses sound waves (ultrasound) to create images of the heart. A Doppler test uses sound waves to measure the speed and direction of blood flow. By combining these tests, a paediatric cardiologist gets useful information about the heart’s anatomy and function.
Kidney Function Test or Glomerular Filtration Rate (GFR) is a test to check to see if kidneys are functioning correctly whilst on chemotherapy. A radioactive injection is given based on the height and weight of your child or sibling. An hour after the injection is given a blood test is taken, then another hour after that (so two hours after the injection) more blood is taken.
The blood is taken and put through a machine which spins and separates the blood. The red blood goes to the bottom and the yellow goes to the top. It is the yellow blood which is tested. This test is not painful, it does however take a few hours.
A pulmonary function test (PFT) is a set of diagnostic tests used to evaluate your child’s or sibling’s lung function or to measure any change in lung health as often the chemotherapy drugs used to treat brain cancer can cause damage to the lungs and breathing.
Spirometry is one of the most common types of pulmonary function tests and is performed by blowing into a plastic tube. The test measures how much air a child can exhale in a single breath and how fast the air comes out. It is especially helpful for determining whether there are any blockages in the airways that impair breathing.
Lung volume tests measure the total amount of air that your child’s or sibling’s lungs can hold. This test, too, involves breathing through a plastic tube. This test is most conducted sitting in an enclosed space which is like a telephone booth. This test can measure pressure differences when taking a big breath, breathing short quick breaths or sometimes when not done in the booth by breathing a mixture of air and a very small and completely safe amount of helium, and measuring the concentration of helium at various points in the process.
Other tests that can be performed are:
Dental Check, Hearing Tests, PPD (Purified Protein Derivative) Skin Test, Nutritionist Evaluation, Psychologist Evaluation, Urine Tests, Chest X-Rays, Cognitive Neuroscience Studies and General Physical Examinations.
Distraction Ideas for Before or During Procedures
Distraction techniques for infants under six months:
- rocking, stroking their face, gentle patting
- having family present
- rattles or other baby toys
- singing
- sucrose and breast or bottle feeding
Distraction techniques for toddlers (six months to two years):
- blowing bubbles or a windmill
- toys and books that make noise or with buttons to push
- singing your child’s favourite song
- light-up toys
- reading a book.
Distraction techniques for older children:
- big belly breathing, blowing away the scary feelings or blowing away the hurt
- blowing bubbles or a windmill
- counting games
- reading a book, or a search-and-find book
- mind pictures, e.g., think about a favourite sport, family holiday, school game or activity; let your child tell a story or answer questions about what is pictured in their mind.
Distraction techniques for adolescents:
- listening to music with headphones
- let them have a choice about parental presence and hand holding
- mind pictures, e.g., think about a favourite sport, family holiday, school game or activity; let them tell a story or answer questions about what is pictured in their mind
- read a book
- relaxation and breathing techniques
- use humour or talk about something unrelated to their procedure
- watching a favourite movie/show or playing a game on a phone or tablet.
(An older child or an adolescent may want to know what’s happening or they may prefer to focus on an activity instead. Some children want to watch the procedure as it happens.)
















